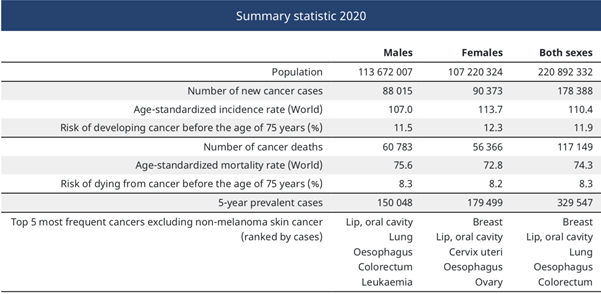
Cancer is one of the leading causes of death in Pakistan1 and around the rest of the world.2; occurred about 178,388 new cancer cases with 117149 cancer deaths in Pakistan in 2020.3 The process of uncontrolled proliferation of normal or previously healthy body cells could resultantly disrupt the normal function of the tissue they reside in, spreading to adjacent and ultimately to distant tissues is known as cancer.
There are about 35 different types of cancers with breast cancer being the most prevalent cancer type among women and lung cancer as the most prevalent cancer type in men in Pakistan.3 Signs and symptoms of almost all types of cancers usually occur at a later stage, when cancer has spread to other organs, majorly contributing to disease-related mortality. One of the most common symptoms of almost all types of cancers including breast and lung cancer is chronic pain.5
Chronic pain and its incidence
An ongoing pain lasting for more than about 12 weeks despite medication intake is known as chronic pain.6 Chronic cancer pain can occur due to cancerous cells pressing against the nearby nerve, bone, or toxins produced by cancerous cells.7 Occurrence of chronic pain can be one of the first signs and symptoms of cancer, requiring careful examination to rule out further the malignancy, the site, and the stage of cancer.7
Chronic pain has been estimated to be prevalent in about 37.3 % of developing countries, including Pakistan.8 It is looked upon as a disease in itself due to its strongly associated biophysical components such as depression, sleep disorders, and functional impairment.9
Chronic pain is a significant factor behind the decline in people’s well-being, social relationships, and ability to live independently. It also leads to a decline in people’s productivity posing to be a major constraint on the economy of the country,10 categorizing it as a major health cause burdening the economy of developed countries like Denmark, the United States of America, and the United Kingdom, etc.11-13
Unfortunately, Pakistan faces the challenge of a lack of up-to-date research on the subject, keeping the experts and policymakers unaware of the significance of chronic cancer pain on the country’s economy and its healthcare. Since the past few decades, chronic cancer pain in Pakistan has been managed as per the WHO guidelines through opioids.
Drawbacks of conventional “opioid therapy” and how the usage of “nerve blocks” can overcome them
Opioids are a form of medicine that previously used to be made from opium poppy but are now human-made in the lab. Opioids depict the effect of natural pain-relieving substances such as endorphins produced by the body and are known to be essentially a part of the pain-management plan for cancer patients.14 However, prolonged use of opioids is accompanied by serious side effects, including breathing and urinating problems plus mental impairments.14
Hence, the researchers’ focus shifted towards deepening their understanding of cellular and molecular mechanisms of pain and developing less harmful and more promising pain-management therapeutics. This led to researchers’ attention at Shaukat Khanum Memorial Cancer Hospital and Research Center being caught by “nerve blocks.” Nerve blocks (nerve blockade) is the intentional interruption of signals traveling along a nerve to fulfill the purpose of pain relief. To study this intervention’s therapeutic efficacy in a clinical setting, a retrospective study15 was launched at the Shaukat Khanum Memorial Cancer Hospital and Research Center in 2016.
The study comprised 252 patients divided into two groups, i.e., cancer patients and non-cancer patients—the cancer group comprised 168 patients with a mean age of about 50 years. Three main interventional procedures were carried out in the study: Coeliac plexus, Epidural Rhizolysis, and Intrathecal neurolysis. Coeliac plexus was performed in patients with upper abdominal organ carcinomas based upon the promising results of a recent study investigating its effect in such patients. Epidural Rhizolysis was carried out for patients with chronic back pain due to its well-established therapeutic role in treating back pain.16-18 Intrathecal neurolysis was used for intractable cancer pain.

The Numerical Rating Scale (NRS) was used to evaluate pain to determine the respective intervention dose and evaluate patient satisfaction one and four weeks post-procedure. The study reported promising findings, with 74.4% of the patients being satisfied with the intervention’s therapeutic effects after one week and 66.07% were satisfied after four weeks of the procedure, whereas 10.12% lost follow-up 4 weeks post-procedure.
Limitations of present research and future implications of “nerve blocks”
Despite the promising findings reported, the study had limitations of small sample size, limited follow-up time of four weeks only, and problems with participant adherence to the study and its protocols. The study did not mention the intervention’s safety profile, nor did it report any drug-related adverse reaction in the participants. The missing data could potentially downgrade the scientific validity of the study results. Hence, a large-scale study with long-term follow-ups of at least 6 months to one year of the study participants with a strategic approach towards patient adherence is warranted.
A well-established safety profile for the intervention can be achieved through the long-term follow up of study participants. Once the research’s highlighted gaps are overcome, the intervention could potentially progress towards seeking approval for its clinical use from the Drug Regulatory Authority of Pakistan as an adjuvant to pharmacological therapy. This would potentially help reduce nationwide opioid usage consequently limiting its health side-effects and economic burden on a country’s healthcare.
References:
- Cdc.gov. 2020. Available from: https://www.cdc.gov/globalhealth/countries/pakistan/pdf/pakistan_factsheet.pdf
- Global Cancer Observatory. Gco.iarc.fr. 2020. Available from: https://gco.iarc.fr
- https://gco.iarc.fr/today/data/factsheets/populations/586-pakistan-fact-sheets.pdf
- NCI Dictionary of Cancer Terms [Internet]. National Cancer Institute. Available from: https://www.cancer.gov/publications/dictionaries/cancer-terms
- Signs and Symptoms of Cancer | Do I Have Cancer? [Internet]. Cancer.org.Available from: https://www.cancer.org/cancer/cancer-basics/signs-and-symptoms-of-cancer.html
- Chronic pain [Internet]. Nhsinform.scot. 2021. Available from: https://www.nhsinform.scot/illnesses-and-conditions/brain-nerves-and-spinal-cord/chronic-pain
- Causes and types of cancer pain | Coping with cancer | Cancer Research UK [Internet]. Cancerresearchuk.org. Available from: https://www.cancerresearchuk.org/about-cancer/coping/physically/cancer-and-pain-control/causes-and-types
- Tsang A, Von Korff M, Lee S, et al.: Common chronic pain conditions in developed and developing countries: gender and age differences and comorbidity with depression-anxiety disorders. J Pain. 2008, 9:883-891. 10.1016/j.jpain.2008.05.005
- Chronic Cancer Pain Management [Internet]. Practical Pain Management. Available from: https://www.practicalpainmanagement.com/pain/cancer/chronic-cancer-pain-management
- Dagenais S, Caro J, Halderman S. A systematic review of low back pain cost of illness studies in the United States and internationally. Spine 2008; 8: 8–20.
- Dagenais S, Caro J, Halderman S. A systematic review of low back pain cost of illness studies in the United States and internationally. Spine 2008; 8: 8–20. [PubMed] [Google Scholar]
- Maniadakis N, Gray A. The economic burden of back pain in the UK. Pain 2000; 84: 95–103. [PubMed] [Google Scholar]
- Swedish Council on Technology Assessment in Health Care (2006). Methods of Treating Chronic Pain. Report No: 177/1+2. http://www.sbu.se/upload/Publikationer/Content1/1/chronic_pain_summary.pdf (accessed 15/08/2008).
- OxyContin Addiction, Abuse, and Symptoms | Help.org [Internet]. Help.org. Available from: https://www.help.org/oxycontin-addiction/
- Ahmad U, Abbas S, Hamadani S, Abbas S, Usman S, Hafeez Z et al. Pain Intervention for Cancer and Non-cancer Pain: A Retrospective Analysis of Tertiary Care Hospital Experience. Cureus. 2020;.
- Nagels W, Pease N, Bekkering G, Cools F, Dobbels P: Celiac plexus neurolysis for abdominal cancer pain: a systematic review. Pain Med. 2013, 14:1140-1163. 10.1111/pme.12176
- Burton AW, Rajagopal A, Shah HN, Mendoza T, Cleeland C, Hassenbusch SJ III, Arens JF: Epidural and intrathecal analgesia is effective in treating refractory cancer pain . Pain Med. 2004, 5:239-247. 10.1111/j.1526-4637.2004.04037.x
- Jeon YS, Lee JA, Choi JW, et al.: Efficacy of epidural analgesia in patients with cancer pain: a retrospective observational study. Yonsei Med J. 2012, 53:649-653. 10.3349/ymj.2012.53.3.649.
Also Read: Defying the odds; Emmanuelle Charpentier & Jennifer A. Doudna

A BSc Human Genetics and MSc Clinical Trials graduate from University College London. An ambitious clinical scientist who is interested in the field of cancer research and keen to promote cancer awareness and improve its therapeutics through her work in the field.