Everyone, at some point in their lives, is introduced to a survivor who has suffered through the dreadful ailment – Cancer. Or we may have lost our loved ones and before death, observed them tread through a path that no one wishes to walk. Countless times, we wished to end their suffrage, but at a certain point, everything must be left to fate. In this age of advancement and technological innovation, it is hard to believe that no proper escape from cancer is available yet (with few exceptions). But one area has caught the attention of researchers and scientists who believe it to be the getaway from cancer: Immunotherapy.
Before jumping on what it is, let’s take a minute to appreciate the human body. You don’t have to be a biologist to be able to praise its delicacy and complexity. The human body is beautiful indeed, how nature has endowed us with complete systems to maintain our existence. From growing into an adult to consuming food to making complex decisions, it is a wonder how intricately interconnected these systems are with each other. Anything goes wrong, and our defense system jumps in to revert everything to normal. But as the saying goes: Nothing is perfect. Sometimes, our cells change so drastically that they can’t stop multiplying, and this uncontrolled abnormal growth is what we call ‘Cancer.’
The Body Patrol
Over the years, many treatments have been suggested, tried, and tested. But few seem to work given that certain circumstances are provided. Cancer cells are so smart and highly advanced that it is a daunting task to treat them. Cancer is killing millions of people each year; it is a health challenge, complicated to tackle. After trying different treatments, scientists have stumbled upon the powerful weapon we all have; our immune system. Present throughout the body, it gives us resistance and fights harmful infectious agents and diseases. At times we don’t even know about all the battles taking place inside our bodies.
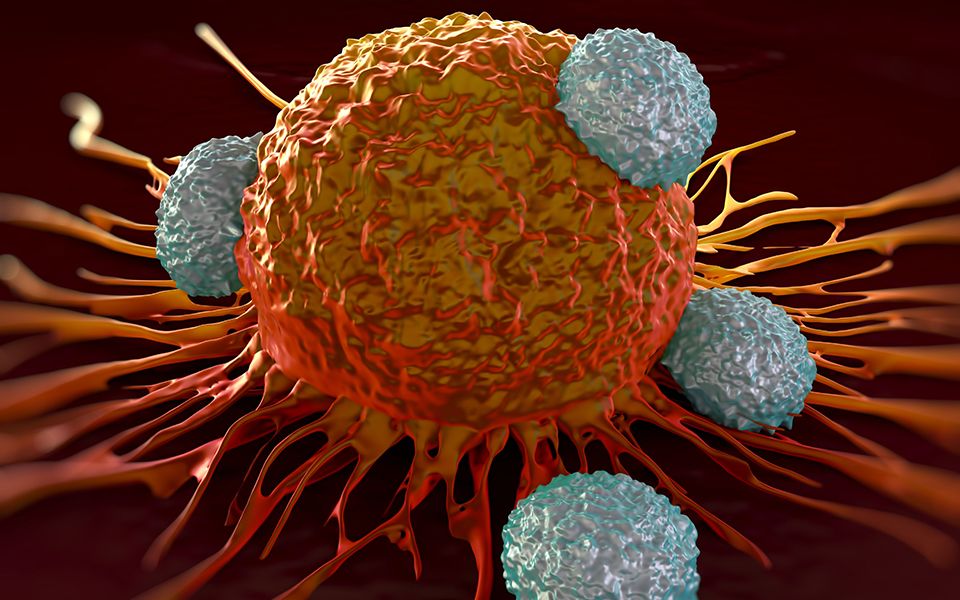
One is inclined to think that if it’s efficient, then why cancer cells escape our immune system in the first place? Well, that is because, as mentioned, they are very clever and are our body’s mutated cells, they aren’t recognized as a foreign threat by the immune system. As they progress and develop, they gain the ability to dodge, fight, and gain control over the defenses. Immunotherapy is such a treatment that seeks to trigger and restore the immune system to recognize and confront cancer.
How it works
Certain parts of the immune system are used in various ways to target cancer cells. Either simulation or recognition abilities are provided to make them work par cancer or components are given that aid in the process of destruction. It may vary according to the different types and may work better for some than the others.
In the case of the detection of harmful agents, the body also makes proteins called antibodies that attack specific parts on an infected cell. These ‘monoclonal antibodies’ can be used to mark cells that can then be degraded by the immune system.
Our immune system’s ability to discriminate between native and foreign cells mostly involves T cells, which are a type of white blood cells. There are accelerators and brakes (yes, just like that in the cars) that modulate a balance so that only foreign cells are killed, and no autoimmune destruction of the standard cell occurs. These are manipulated by cancer cells so that they can remain incognito.

In immunotherapy, drugs are used to release these brakes leading to wipeout of dangerous cells. The Noble Prize in Physiology or Medicine 2018 was awarded to scientists James P. Allison and Tasuku Honjo, who discovered the crucial pathways i.e. PD-1 and CTLA-4 that cancer cells use to escape. But by blocking these pathways with antibodies, a response is restored. This treatment is called ‘immune checkpoint therapy.’
Another type of T-cell therapy includes targeting receptors. These are the proteins present on the cell surface which help in recognition, signal transmission and are basically the “eyes and ears of the cell.” Altering the receptors in the cell makes them efficiently recognize cancer cells which are then sought from the entire pool and degraded. This therapy is called Chimeric Antigen Receptor (CAR) T-cell therapy and has been helpful in certain blood cancer treatments. Scientists are researching to understand it better and develop effective therapies.
Non-Specific Immunotherapies are another class that aids the immune cells in their quest to destroy cancer. These can be given during other cancer treatments (such as radiation and chemotherapy) or after their completion. Most common include Interferons and Interleukins. The former slows down and hinders the growth of cancer cells and the latter helps in the production of those that are involved in the fight. The medicinal treatments also have drawbacks as well which may vary from person to person, but common side effects include hair loss, high risk of infection, weight gain, low blood pressure, etc.
Expectations vs. reality
All this sounds very impressive and using one’s defense system is a great idea, but has its limitations and problems. While some may be cured on a miraculous level or experience an everlasting response, other patients may not respond that well to immunotherapy. The majority don’t receive a positive effect and studies have shown that the response rate is 20% with a varying survival rate. To find which cancers are the best enemies of this therapy, extensive research is being conducted and methods are being identified. New immunotherapy approaches include improvements through nanotechnology, precision therapy and many more.

Image Credit: HYACINTH EMPINADO/STAT
Those who receive it may go through drastically different phases: fine at first, sick later. New side effects may originate confusing both the doctors and patients, and severe toxicities startle researchers. This ‘trial and error’ situation is depressing but necessary. Pressure from big pharma and medical industry to develop effective drugs and treatment against cancer is high leading to the conduction of thousands of trials (in which participation rates also drop now and then) where the researchers aim to explore and find the expectations of others suppress an answer. Challenges arise for oncologists who not only have to work out solutions but also have to convince patients who demand immunotherapy without being aware of its pros and cons, just because they have heard about its miracles.
But this shouldn’t lead to the conclusion that it is rouge role outperforms the benefits. There are success stories as well, and various research institutes around the world are leading the way. Who knows, it may even beat out conventional chemotherapy. But a reality check can help to keep things in place and create a balance between the trend and its potential. Immunotherapy surely has the potential to alter the landscape of cancer treatments and deserves all the praise and attention. It has a long way to go, but hope should keep alive for it can indeed change and save lives of millions of people who have cancer, a feat yet to accomplish.
Did you like that? Then check out The Taboo around Cancer in Women

Maham Maqsood is a science communicator and co-founder at Scientia Pakistan. She is currently doing Masters in Biochemistry at the Middle East Technical University, Turkey. She has over five years of experience in science communication and outreach, collaborating with researchers, educators, and communicators to develop effective strategies and content for various platforms and events.