Once as a child, I developed a raging fever and rash all over my body. My parents rushed me to a nearby hospital. The doctor diagnosed me with scarlet fever and prescribed some antibiotics. I remember him telling me that long ago, people used to die of this fever, but I’m lucky enough to be born in an antibiotic era.
I took that antibiotic regularly, and I got cured of an incurable disease for decades.
We all have taken antibiotics, but what if antibiotics never existed?
History contains lessons from the pre-antibiotic era when most people failed to combat bacterial supremacy. Scientists predict that within the next 20 years, we will be in the post-antibiotic age, where something as small as a cut could be lethal. All thanks to the superbugs.
Let’s find out what superbugs are and how they are turning the course of history by creating antibiotic resistance.
How do antibiotics fight bacteria?
Bacteria behave differently in the human body; utilizing these differences in several components of the bacterial structure, the bacteria can be easily targeted by certain chemicals (antibiotics) without harming humans.
Antibiotics work like a key in a lock by specifically disrupting these components leading to the inactivation of bacteria. Hence, making them less of a threat. Exposure to antibiotics kills most of the bacteria, yet some survive the treatment and evolve into the super strong stragglers known as superbugs.
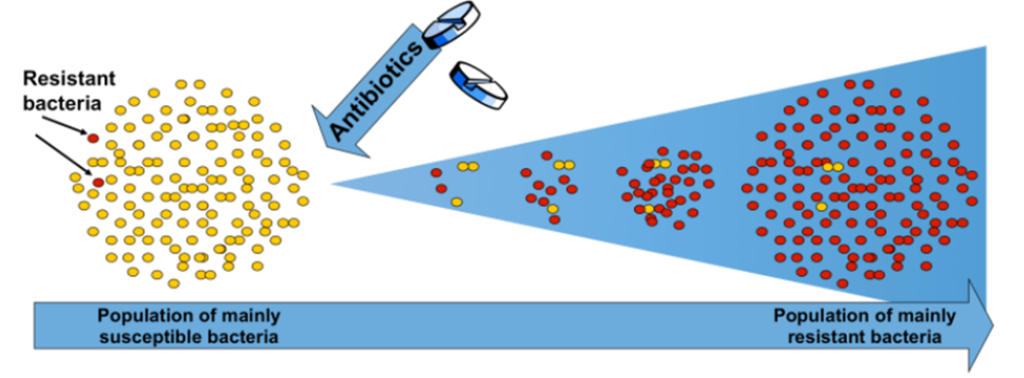
Let’s discover how bacteria have mastered this art of survival.
Evolution of resistant bacteria
Life finds a way!
Being the first life on earth, bacteria have undergone creative evolution, making themselves the most intelligent creatures with superpowers. These superbugs were developed when repeated antibiotics exposure allowed the bacteria to play smart and adopt the below-mentioned mechanisms to cope with the attack.
Natural resistance
Some bacteria naturally possess defense mechanisms against antibiotics. This intrinsic trait appears to be independent of previous antibiotic exposure. These bacteria exhibit defense in two ways:
- Sometimes, the antibiotics latch onto the bacterial surface to attack. In contrast, bacteria counteract this by changing their structure to become unrecognizable from the drug.
- The other way bacteria defend themselves is by releasing chemicals to destroy the antibiotic molecule.
Horizontal gene transfer (HGT)
Just like humans, bacteria also possess DNA, the blueprint of cells. The DNA contains a message to make proteins that further form the cells, organs, and, ultimately, the entire organism.
Horizontal gene transfer allows the bacteria to receive DNA/genes from already resistant bacteria or viruses. The genetic material (DNA/gene) of a resistant bacterium contains a message for resistance, giving it a competitive advantage in survival against antibiotics.
This process can be done in three different ways:
- Transduction
Some viruses, known as bacteriophages, can attack bacteria. During the attack, bacteriophage takes some portion of bacterial DNA (with resistance) and sneaks out.
Later this bacteriophage attacks and drops off the stolen DNA into another bacterium making it resistant too.
- Transformation
Sometimes resistant bacteria release their DNA into the extracellular environment. Hence, the other bacteria in the surrounding absorbs the free, resistant DNA and add it to their genetic information.
- Conjugation
This process allows DNA transfer between two bacteria by direct cell-to-cell contact or a bridge-like connection. The resistant DNA transfer enables the recipient bacteria to make proteins responsible for antibiotic resistance.
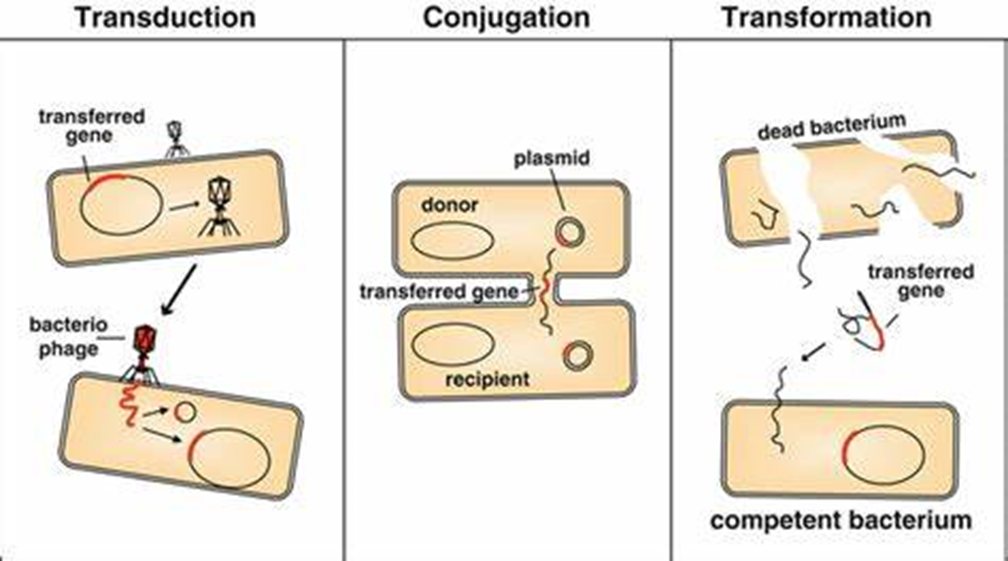
Genetic mutation
Unlike humans, bacteria reproduce by making copies of themselves (multiplication). Sometimes while copying their DNA, bacteria create a random mistake (mutation), producing a different DNA (mutant DNA) than the original. At times, the mutant DNA contains resistance allowing the bacteria to bypass the action of antibiotics.
Let us now discuss how humans have facilitated the rise of superbugs.
How do humans create superbugs?
Do you know that humans also help superbugs in building their resistant legacy?
Some of our standard practices are leading us to the global health crisis, such as:
- Misuse of antibiotics against viral infections. This negligence results in no cure but the survival of resistant bugs instead.
- Moreover, it is also essential to complete the antibiotics course.
As we take antibiotics, the bacterial population is reduced, making us feel better. That’s when we decide not to complete the antibiotic course. As a result, some bacteria in the body referred to as ‘persisters’ (as they persist…obviously) start to grow and cause a recurrent infection that turns out to be worse.
Now, would you allow yourself to feel the same all over again after knowing what you know?
How antibiotic resistance enters the food chain?
Antibiotics are called ‘the societal drugs’ because their individual use affects the community and the environment.
You will be shocked to know that the largest consumer of antibiotics is the agriculture industry. Here the use of antibiotics is not just to limit the infection in food animals but also, to promote their growth.
This is a problem because many bacteria are common among animals and humans (can infect both species), like Salmonella. Therefore, the resistant strains can easily pass us through the food chain. Indeed, this spread widens to the global level through international trade and travel networks.
Today many bacteria are resistant to all currently available drugs on the market, leading us to the post-antibiotic era.
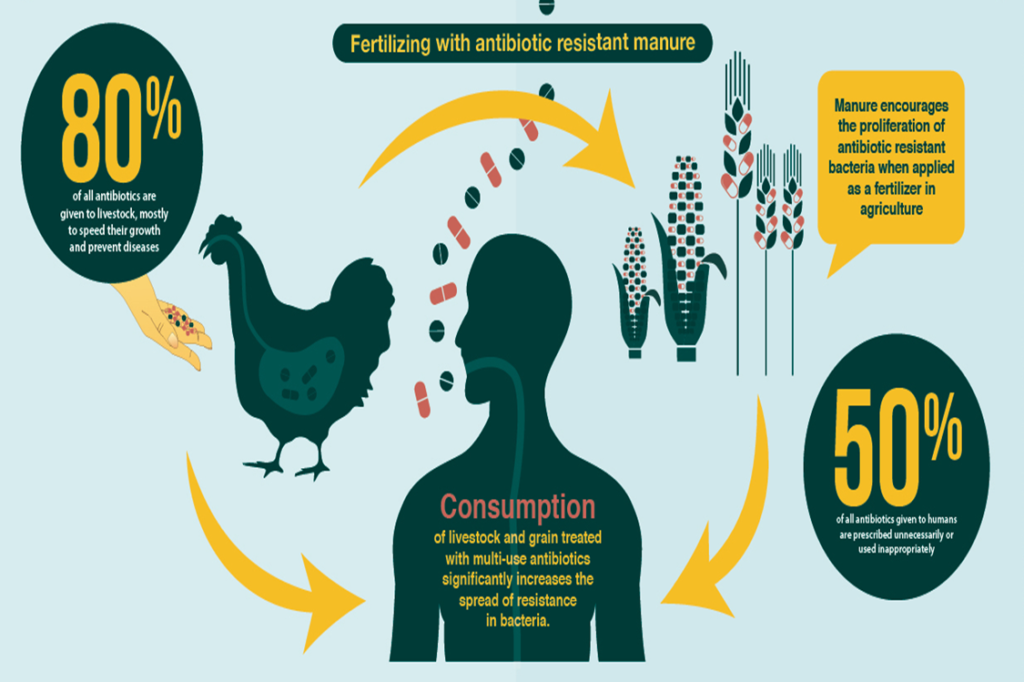
Wondering how you can help tackle this problem?
Time to fight back!
We can fight health threats through the prudent use of antibiotics. Scientists are continuously getting to the grips to stem antibiotic resistance. Many alternative options are being explored, such as bacterial vaccines and phage therapy which uses viruses with the ability to infect and kill bacteria.
However, more research is required to halt the progression of antibiotic-resistant bacteria.
If humanity plays its card right, the superbugs’ superiority can be challenged.
Learn more about yourself by being close to science.
References:
- Reygaert W. C. (2018). An overview of the antimicrobial resistance mechanisms of bacteria. AIMS Microbiology, 4(3), 482–501. https://doi.org/10.3934/microbiol.2018.3.482
- (n.d.). Tackling antibiotic resistance – testing shows signs of progress. Animal and Plant Health Agency. https://aphascience.blog.gov.uk/2020/08/01/tackling-antibiotic-resistance/
- (n.d.). Antimicrobial Resistance. Centre for Disease control and prevention. https://www.cdc.gov/drugresistance/about.html
- Levy, S. B. (1998). The Challenge of Antibiotic Resistance. Scientific American, 278(3), 46–53. http://www.jstor.org/stable/26057703
- (n.d.). Antibiotic Resistance: An Old Solution but a New Problem. https://blog.addgene.org/antibiotic-resistance-an-old-solution-but-a-new-problem
Also, Read: The Truth about the Role of Bioterrorism and Conspiracies in the Pandemics

Huda Munawar is a Bioscientist, currently doing her masters in Healthcare Biotechnology from NUST. She aims to bridge the gap between scientific community and the public through her writing.

